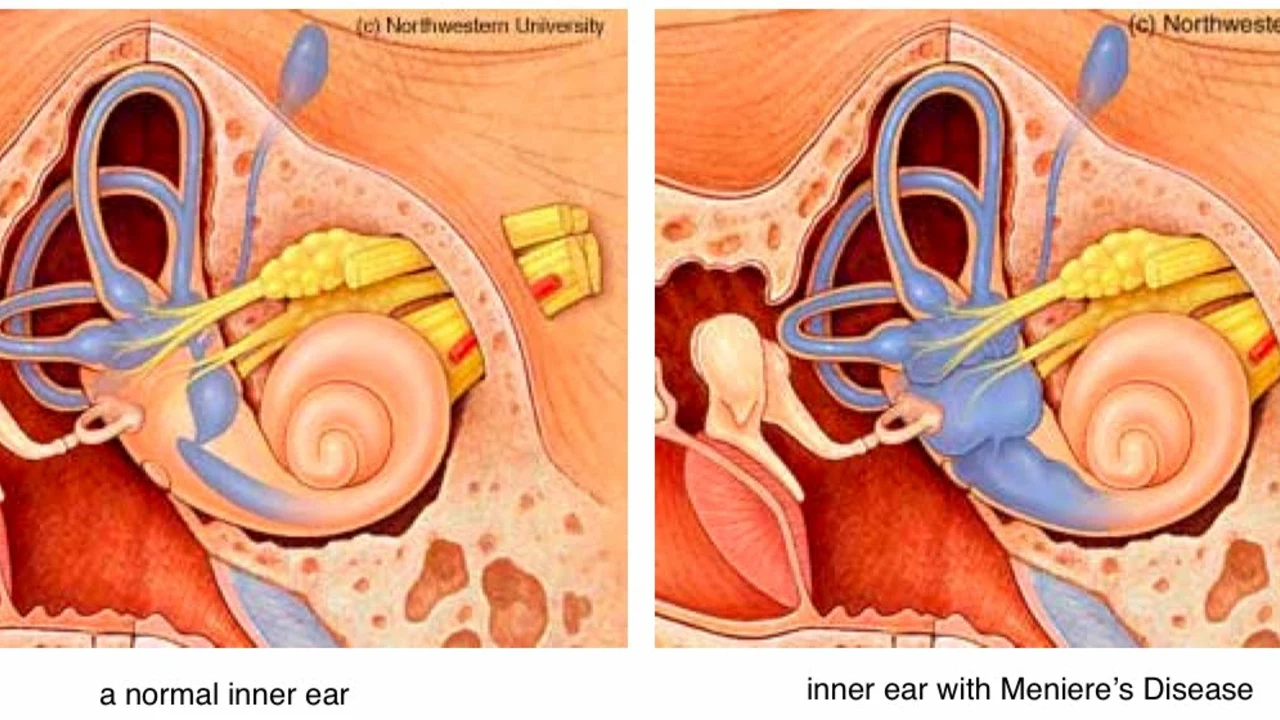
Meniere's disease — symptoms, causes, and what you can do now
One severe vertigo spell can last hours and leave you drained for days. If you get repeated attacks of spinning, ringing in the ear, and a feeling of fullness, Meniere's disease might be the cause. This page gives clear, practical steps you can use today and what to expect from doctors.
What to watch for
Typical signs are sudden, strong vertigo that lasts 20 minutes to several hours, fluctuating hearing loss (often low tones first), tinnitus (ringing or buzzing), and a full or blocked feeling in the ear. Symptoms tend to come in episodes. Between attacks you may feel normal, but hearing can slowly get worse over time.
If you have nausea, vomiting, or can't stand during an attack, treat the situation like a medical emergency only if symptoms don't ease or if you have new neurological signs like weakness, double vision, or trouble speaking.
Causes and diagnosis
Meniere's is linked to extra fluid in the inner ear (endolymphatic hydrops). Why that fluid builds up isn't fully clear—possible triggers include viral infection, impaired fluid drainage, immune issues, or a history of head trauma. Some people have migraine-related patterns that look like Meniere's.
Doctors diagnose it with a medical history, hearing tests (audiogram), balance tests (ENG/VNG), and sometimes an MRI to rule out other issues. Keep a symptom diary—dates, duration, triggers, and how severe the attack was. That helps your clinician make a clear diagnosis faster.
What works for one person may not work for another. Treatment focuses on reducing attack frequency and protecting hearing.
Practical steps to reduce attacks
During an attack: sit or lie down in a dark, quiet room, focus on a fixed point, and avoid sudden head movements. Over-the-counter or prescription anti-vertigo meds (like meclizine) and anti-nausea drugs can help short-term—check with your provider first.
Daily habits that often help: follow a low-salt diet, limit caffeine and alcohol, stay hydrated, and manage stress and sleep. Many ENT doctors also recommend vestibular rehabilitation (specific balance exercises) to speed recovery between attacks.
Medical options include diuretics, intratympanic steroid injections, or gentamicin injections (which reduce vertigo but risk hearing loss). Surgery is considered when other treatments fail—options range from sac procedures to vestibular nerve section. Hearing aids and, in severe cases, cochlear implants can help persistent hearing loss.
See an ENT if you have repeated spells, rapid hearing decline, or attacks that stop you from daily life. Keep notes, ask about hearing tests, and discuss both medical and lifestyle choices. With the right plan, most people reduce attacks and improve quality of life.